Preventing medication errors is all about having a clear, organized, and loving plan. It comes down to creating one complete and accurate medication list, setting up smart and simple storage, and communicating clearly with doctors and pharmacists. This approach can turn what feels like an overwhelming task into a safe, manageable routine for the person you love.
The Heart of Caregiving Is Keeping Them Safe

If you've ever walked out of a hospital with a loved one, clutching a bag full of new prescriptions and a stack of discharge papers, you know that feeling. It's a mix of relief that they're finally coming home and a wave of anxiety about the new responsibilities suddenly on your plate.
You might find yourself wondering, "Did I catch everything the doctor said? What if I mix up these new pills with the ones they were already taking?"
Please know this feeling is completely normal. You are not alone. Being a caregiver is one of the most profound acts of love, and managing medications is one of its most critical duties. The good news is, you don’t have to be a medical professional to do it safely and effectively.
Why This Matters So Much
The reality is that medication errors can happen at any stage—from the doctor's office to the pharmacy to your own kitchen counter. These mistakes are a leading cause of preventable harm in healthcare, with global costs estimated at a staggering $42 billion every year.
Most of these errors aren't due to a lack of love or care, but to system issues, simple distractions, or honest human error. You can learn more about this global health initiative from the WHO. This is exactly why having a clear, simple plan is so important. It protects your loved one and brings you some much-needed peace of mind.
This guide is your roadmap. We’ll walk through practical, step-by-step strategies designed for real families. Our goal is to replace that feeling of anxiety with quiet confidence, empowering you with the tools to manage medications safely and calmly.
This journey is about creating simple, reliable systems that make the right choice the easiest choice. You have what it takes to protect the person you care for, and we're here to support you every step of the way.
Your first small step: Take a deep breath. Just by seeking out this information, you're already showing how much you care.
Create a Medication Master List for Total Clarity

If you’re trying to prevent medication errors, the single most powerful first step you can take is creating one accurate list of every single thing your loved one takes. This isn’t just about prescriptions; it’s about getting a complete picture of everything they put into their body.
This process, sometimes called medication reconciliation, is how you turn a jumble of pill bottles and confusing instructions into a clear, manageable plan. It becomes your family’s single source of truth—a document you can rely on during doctor’s visits, hospital stays, and daily care.
Think of it as your roadmap to safety and peace of mind.
Start by Gathering Everything
Your first move is simple: gather it all up. Go through the medicine cabinet, check the kitchen counter, look on their bedside table, and don't forget to check their purse or bag. You're looking for absolutely everything.
This includes:
- All prescription medications from every single doctor (cardiologist, primary care, specialist).
- Over-the-counter (OTC) drugs like pain relievers, allergy pills, or antacids.
- Vitamins, minerals, and supplements such as Vitamin D, calcium, or fish oil.
- Herbal remedies like St. John's Wort or Ginkgo Biloba.
- Any creams, ointments, or eye drops that contain active medication.
It can feel like a bit of a treasure hunt, but this step is non-negotiable. Many seemingly harmless supplements or OTC products can interact dangerously with prescription drugs. Having them all in one place gives you the full, unvarnished picture.
A Real-World Scenario: Sarah’s Story
Let’s imagine Sarah, who just brought her father home from the hospital after a heart procedure. The hospital gave him three new prescriptions, but she also has all his regular medications from his primary care doctor. She feels that familiar knot of anxiety, worried she might miss something important.
Instead of guessing, Sarah sits down and creates a master list. She lays out all the bottles—new and old—and starts writing everything down. As she does, she notices the hospital discharge papers say to stop taking one of his old blood pressure pills, but the bottle from his local pharmacy was just refilled.
Without her master list, she might have continued giving him both, risking a dangerous drop in his blood pressure. This simple act of reconciliation caught a potentially serious error before it could happen.
This kind of confusion is incredibly common, especially for older adults. In fact, people prescribed five or more medications face a 30% higher risk of medication errors, and that risk climbs to 38% for those over 75. These risks are highest during transitions like a hospital discharge, where clear communication can sometimes break down.
Documenting the Details That Matter
Now, let's turn that pile of bottles into an organized, powerful tool. You can use a simple notebook, a spreadsheet, or a dedicated app. For a user-friendly option, the Don'tForgetDad Android app can help you not only list medications but also schedule reminders for each one.
No matter what tool you use, here’s a simple template to make sure you capture all the essential information. Bring this list to every single doctor's appointment.
Your Medication Master List Template
| Medication Name (Brand & Generic) | Dosage (e.g., 50 mg) | How Often to Take | Reason for Taking | Prescribing Doctor | Special Instructions |
|---|---|---|---|---|---|
| Lisinopril (Prinivil) | 10 mg | Once daily in the morning | High blood pressure | Dr. Evans (Cardiologist) | Take with food |
| Metformin | 500 mg | Twice daily with meals | Type 2 Diabetes | Dr. Smith (Primary) | Avoid alcohol |
Make sure to fill out every column for every single medication, vitamin, and supplement. This detailed view is what helps you and the doctors spot potential issues.
Once your list is complete, make copies. Keep one with your loved one’s medications, carry one in your bag, and give one to another trusted family member. This document is now your most important tool for every medical visit.
This master list does more than just organize information; it empowers you. It turns you from a passive recipient of instructions into an active, informed partner in your loved one’s care.
Your next small step: Block out 30 minutes this week. Gather all the medications in one place and start your list. Just getting started is a huge win.
Organize and Store Medications for Maximum Safety
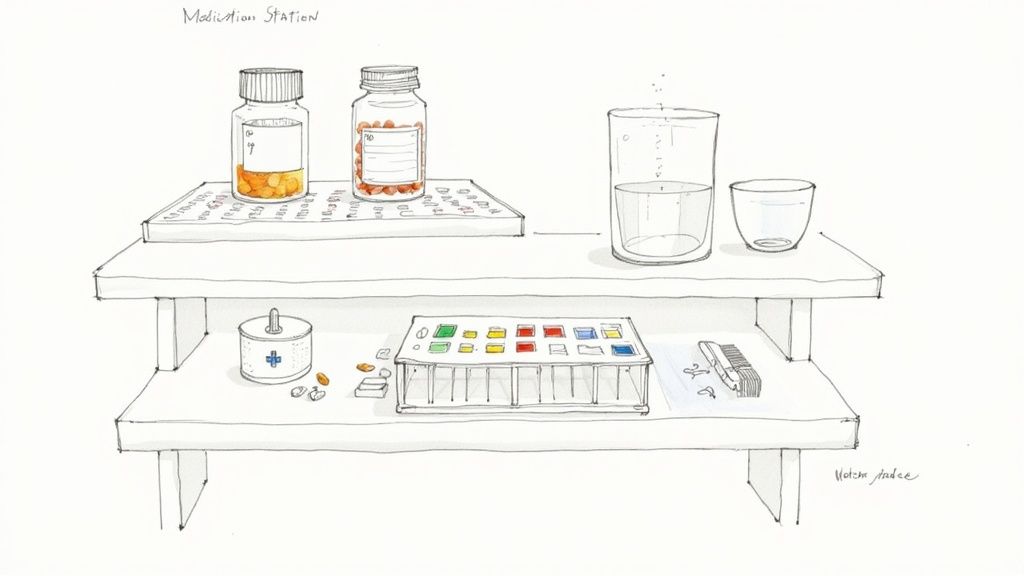
Now that you've built your Medication Master List, you have the blueprint for safety. The next step is to bring that same level of intention and order right into your loved one's home. A smart storage system does more than just clear up counter space; it creates an environment where the right choice is always the easiest one.
This is about moving beyond the standard advice to "store in a cool, dry place." We're going to create a practical, real-world system that actively prevents medication errors before they even have a chance to happen.
Choosing the Right Tools for Your Family
Every family's situation is unique, so the best tool is the one that fits your actual life. For many, a simple weekly pill organizer is the perfect place to start. It lets you set up all the medications for an entire week at once—a huge time-saver and an even bigger stress reducer.
If your loved one has a more complex schedule or is dealing with memory challenges, an automated pill dispenser might be a better fit. These devices can be programmed to dispense only the correct pills at the right time, usually with a loud alarm. Some can even send a text alert to a caregiver's phone if a dose is missed.
- Weekly Pill Organizers: Ideal for simple, consistent schedules. They give you a quick visual check to see if today’s dose has been taken.
- Automated Dispensers: A great option for those with cognitive decline or very complicated medication regimens. They add an essential layer of security.
- Blister Packs from the Pharmacy: Many pharmacies will pre-package medications into daily or weekly blister packs, taking all the sorting work off your plate.
The key is to pick a system you can all stick with. It doesn't have to be fancy, just foolproof.
Conquering Common Household Hazards
Your home is a place of comfort, but it can also hide risks for medication mix-ups. One of the most common—and most dangerous—is simply storing medications that look alike next to each other.
Imagine you're in a hurry to give your mother her morning pills. You reach for her blood pressure medication, but the bottle looks almost identical to her cholesterol pill sitting right beside it. It’s an honest mistake, but one with potentially serious consequences.
Even in highly controlled environments like hospitals, persistent risks like look-alike/sound-alike medications require focused intervention. Simple failures, such as storing similar-looking drugs together or not removing old medications from circulation, can undermine even the best safety measures. Discover more insights from this study about medication safety protocols.
Let’s make sure this doesn’t happen at home. By taking a few simple, intentional steps, you can design a system that makes it easy to grab the right medication, every single time.
Simple Fixes for a Safer Home
Creating a safer medication space is all about small, deliberate actions. You don’t need to completely overhaul the house; just a few thoughtful adjustments can make a world of difference.
Here are some practical, easy-to-implement ideas:
- Separate Look-Alikes: If you have medications with similar-looking bottles or pills, store them on different shelves or in completely separate bins. Physical distance is one of your most powerful safety tools.
- Use Visual Cues: Add a bright-colored sticker or wrap a rubber band around one of the look-alike bottles. This simple visual flag forces you to pause and double-check before you administer the pill.
- Keep Medications in Original Bottles: Always store medications in their original, clearly labeled pharmacy containers. That label contains critical information, including the medication name, dosage, and expiration date.
- Designate One Spot: Create a single, designated “medication station” in a place that is cool, dry, and safely away from children or pets. The bathroom medicine cabinet, with its heat and humidity, is actually one of the worst spots.
These small habits build on each other, creating layers of protection that keep your loved one safe.
The Importance of Clearing Out the Old
Finally, an essential part of safe storage is regularly cleaning out old medications. An expired or discontinued prescription left in the cabinet is a medication error just waiting to happen. Someone could easily grab it by mistake, thinking it's a current prescription.
Set a reminder on your calendar every six months to go through the medication station. Check the expiration dates on everything—including over-the-counter items—and safely get rid of anything that’s old or no longer on the Medication Master List. Most pharmacies offer medication take-back programs that make disposal safe and easy.
Your hopeful takeaway: This week, find two medications in your loved one's collection that look similar. Put a colored sticker or a rubber band on one of them. You’ve just made their daily routine a little bit safer.
Build a Reliable Daily Medication Routine
With your loved one's medications organized and a master list in hand, you're ready for the next powerful step: building a reliable daily routine. Consistency is your absolute best friend when it comes to medication safety.
A predictable rhythm does more than just prevent mistakes; it brings a sense of calm and control to what can often feel like a chaotic part of the day. This isn't about being perfect. It's about creating a simple, repeatable system that lowers stress for both you and your loved one, making safety feel like a natural part of your day.
Making the 'Five Rights' Simple
In hospitals, nurses live by the "Five Rights" of giving medication. It might sound a little clinical, but for a caregiver, it’s really just a simple mental checklist that you can weave into your daily habit. Let's translate these rules into easy, everyday actions.
Right Person: Before you hand over any pill, just glance at the name on the prescription bottle. It takes a single second, but it confirms you’ve got the right person, which is especially important if you’re caring for more than one family member.
Right Medicine: Read the name of the medication out loud from the bottle. This small action forces a tiny pause, helping you confirm you’ve picked up the correct one and preventing mix-ups with those look-alike bottles.
Right Dose: Double-check the label for the dosage. Does it say one tablet or two? Is it 10mg or 20mg? A quick look at your master list will confirm you have the right amount.
Right Way: This just means how the medication is given. Most are pills to be swallowed, but some might be creams, drops, or liquids. Confirming this prevents mistakes like trying to swallow a sublingual tablet that should dissolve under the tongue.
Right Time: Is this the morning dose or the evening dose? Should it be taken with food or on an empty stomach? Sticking to the schedule is crucial for the medication to work effectively and safely.
This five-step check becomes second nature very quickly. It’s not about being rigid; it’s about creating a small, powerful habit that acts as a final safety net for every single dose.
Create a Calm Medication Station
Distractions are a leading cause of medication errors. Rushing around looking for a glass of water, a spoon for liquid medicine, or a pill cutter at the last minute opens the door for mistakes.
The solution is simple: create a calm, dedicated "medication station." This doesn't need to be anything fancy. It can be a small tray on the kitchen counter or a designated corner of a dresser. The key is to have everything you need in one place, ready to go.
Your station should include:
- The pill organizer for the current day or week
- A fresh glass of water
- Any necessary tools like a pill splitter or crusher
- A small cup for applesauce or yogurt if needed to help with swallowing
By setting this up ahead of time, you create a peaceful, focused environment. When it's time to give the medication, you can focus entirely on the task at hand—running through your "Five Rights" checklist without feeling rushed or frazzled.
Think of it like a pilot’s pre-flight check. They don’t skip it because they’ve flown a thousand times. They do it because they’ve flown a thousand times, and they know that consistent, simple checks are what ensure a safe journey.
Using Gentle Reminders to Stay on Track
Even with the best intentions, life gets busy and it’s easy to forget a dose. This is where simple technology can be an incredible ally, providing gentle nudges that keep your routine on track. You don’t need anything complicated.
Your smartphone is already a powerful tool. You can set recurring daily alarms for each medication time, labeling each one specifically (e.g., "Dad's 8 AM heart pill"). A clear reminder like that cuts through the noise of a busy day.
For families coordinating care, a specialized app can be even more helpful. A caregiver support tool like the Don'tForgetDad iOS app allows you to set up schedules and receive notifications if a dose is missed. This creates a shared sense of responsibility and ensures that someone always follows up—an extra layer of safety that provides incredible peace of mind.
Ultimately, building a routine is about layering these simple habits: the five-step check, the calm station, and the gentle reminders. Each one is a small action on its own, but together, they create a strong, reliable system that protects your loved one.
Your hopeful takeaway: Set just one labeled alarm on your phone today for your loved one's most important medication. This simple step is the beginning of a powerful, consistent routine.
Communicate Confidently with Doctors and Pharmacists
As a caregiver, you are your loved one's single most important advocate. You hold a vital position on their healthcare team, and your voice matters—a lot. Still, speaking up in a busy doctor's office or pharmacy can feel intimidating.
It's easy to feel rushed or worry that you're "bothering" them with your questions. Please hear this: Your questions are never a bother. They are one of the most powerful tools you have to prevent medication errors and ensure your loved one gets the safest, most effective care possible.
Your Master List Is Your Conversation Starter
Remember that Medication Master List we talked about creating? It's more than just a piece of paper—it's your script for confident conversations. Instead of trying to recall every detail under pressure, you can simply hand it over at the start of every single appointment.
This immediately gives the doctor or nurse a complete, accurate picture of your loved one’s health. It also shows them you are organized, engaged, and a serious partner in their care.
A caregiver's simple action: Before the doctor even begins the exam, say something like, "To make sure we're all on the same page, here is a current list of everything Mom is taking, including her vitamins and daily aspirin." This one sentence sets a collaborative tone for the entire visit.
From there, any conversation about new prescriptions starts from a place of shared knowledge. You won't be scrambling to recall dosages or names; it's all right there in front of both of you.
Essential Questions for Any New Prescription
When a doctor suggests adding a new medication, that's your cue to gather the critical information that ensures safety at home. Don't ever hesitate to pull out a notebook and jot down the answers. This isn't about challenging their expertise; it's about ensuring you can follow their instructions perfectly.
Here are a few key questions to ask every time:
- What is the name of this medication, and what exactly is it for?
- What specific side effects should I watch for?
- Can this be taken with or without food?
- How will we know if it's working?
- Is there anything on our current list that this could interact with?
Getting this information upfront is a crucial step in preventing errors once you get home.
Your Pharmacist: An Invaluable and Accessible Ally
One of the most underutilized resources for caregivers is the local pharmacist. These professionals are true medication experts, and they are often far more accessible for a quick question than a busy doctor. They can be your final safety check before a new drug ever enters your home.
Think of this real-world scenario:
A caregiver named Mark goes to pick up a new antibiotic for his wife, who is already on a blood thinner. He remembers the doctor mentioned it was safe, but he feels a little nagging doubt. When the pharmacist hands him the bag, Mark decides to ask, "I just want to double-check—this is okay to take with her Warfarin, right?"
The pharmacist pauses and pulls up his wife’s profile. After a moment, he says, "I'm so glad you asked. This specific antibiotic can actually increase the effect of her blood thinner, raising her bleeding risk. Let me call the doctor and suggest a safer alternative."
Mark’s simple, two-second question prevented a potentially life-threatening drug interaction. He wasn't a medical expert; he was just an attentive caregiver who wasn't afraid to speak up. Your pharmacist is there to help you do the same. Never hesitate to use their expertise.
Your hopeful takeaway: The next time you pick up a prescription, just ask the pharmacist one simple question: "Is there anything special I need to know about this?" It opens the door for a helpful conversation and reinforces your role as a proactive caregiver.
What to Do If a Medication Mistake Happens

No matter how careful you are, mistakes can happen. It’s an unfortunate reality of caregiving. The moment you realize an error has been made with a medication, your first instinct might be to panic. Don't. Your calm, clear-headed response is what matters most right now.
That sinking feeling in your stomach—the wave of guilt and fear—can be overwhelming. Take one slow, deep breath. Before you do anything else, check on your loved one. Are they alert? Do they seem different in any way? Their immediate well-being is your only priority.
Your Immediate Action Plan
Once you've assessed them, it's time to get professional guidance. This isn't something to solve on your own or to "wait and see." Every minute can count, and there are experts ready to walk you through it.
Here are the first two calls you need to make, in this order:
Poison Control Center (1-800-222-1222): This should always be your first call. They are available 24/7 and are the true experts in these exact situations. Be ready to tell them the name of the medication, the amount taken, and your loved one's age and approximate weight.
Their Doctor or Pharmacist: After you have instructions from Poison Control, get in touch with their primary care physician or pharmacist. They understand your loved one's full medical history and can give you specific advice tailored to their other health conditions.
Keep these numbers saved in your phone and posted somewhere obvious, like the refrigerator. Having them handy means you won't be scrambling in a moment of stress.
A Note on Self-Compassion
It’s completely normal to feel awful after a mistake. But an error is not a reflection of your love or your worth as a caregiver. You're human, and you're managing an incredibly demanding role.
Instead of getting stuck on blame, try to see this as an opportunity. A mistake shines a bright light on a weak spot in your system—it’s a chance to make your routine even safer. It’s about finding a solution, not finding fault.
This journey is about progress, not perfection. You are doing your best in a tough situation, and that is more than enough.
Your hopeful takeaway: Take a moment right now to add the Poison Control number (1-800-222-1222) to your phone's contacts. It’s a simple two-minute task that brings incredible peace of mind.
Got Questions? We’ve Got Answers.
As you get deeper into caregiving, you’re going to run into some tricky situations. It’s completely normal to have questions when you’re managing something as important as a loved one’s medication. Here are some quick, real-world answers to the challenges we hear about most.
What Should I Do If My Loved One Refuses Their Medication?
This is a tough one, and it happens more often than you’d think. The first thing to remember is to stay calm and approach it with curiosity, not frustration. Try to figure out the why behind the refusal.
Is the pill just too big to swallow? Does it leave a bad taste or make them feel nauseous? Sometimes the solution is surprisingly simple, like asking the pharmacist if it’s okay to crush a pill and mix it into a spoonful of applesauce. You can also try connecting the medicine to a goal they care about: "Mom, this is the pill that keeps your heart strong for when the grandkids visit."
If they still refuse, don’t ever force it. That’s your cue to call their doctor. There might be an alternative available, like a liquid version or a different medication that’s easier for them to tolerate.
How Can We Manage Meds When Multiple Family Members Help?
When you’re sharing caregiving duties, communication is everything. Without a rock-solid system, it’s frighteningly easy for a dose to be missed—or worse, accidentally given twice.
The key is to agree on a single source of truth that everyone updates in real-time. This could be a simple notebook kept right next to the pill organizer, where each person initials a checklist after giving a dose. A shared digital note or a dedicated group chat can also work wonders.
A quick "handoff" conversation can be a lifesaver. When another caregiver arrives, just take two minutes to go over what’s been given and what’s coming up next. This simple act of teamwork makes the whole process so much safer.
What Should I Check When My Parent Is Discharged From the Hospital?
A hospital discharge is one of the most dangerous times for medication errors. It's a whirlwind of new information, and it's easy for things to get missed. Before you even think about leaving, ask the nurse or discharge planner to do a "medication reconciliation" with you. This isn't just a good idea—it's essential.
Bring your up-to-date Medication Master List from home and compare it, line by line, against the hospital’s new discharge instructions. Make them clearly explain what each new medicine is for. And here’s the most critical question you can ask: "Which medications from our home list should we stop taking now?"
Get all of this in writing before you walk out that door. Taking those extra ten minutes can prevent a serious, and completely avoidable, mistake. For more tips on navigating the ins and outs of family caregiving, feel free to explore our other articles on the Don'tForgetDad caregiving support blog.
 by Don'tForgetDad Team
by Don'tForgetDad Team