When your loved one is struggling to catch their breath, their albuterol inhaler isn't just a piece of plastic—it's a lifeline. Knowing the right way to use it ensures that this little device can deliver comfort quickly and effectively, right when they need it most. This guide is here to walk with you through the steps, turning a stressful moment into a calm, confident act of care.
Your Supportive Guide to the Albuterol Rescue Inhaler
Watching someone you care for struggle with shortness of breath is a heavy experience. It can be jarring, whether it's your father getting winded after bringing in groceries or your mother feeling breathless after a short walk. In those moments, your calm, supportive presence can make all the difference. That little blue albuterol inhaler, often called a "rescue" inhaler, is the tool that can help.
Its purpose is simple but powerful. It contains a fast-acting medicine called a bronchodilator, which works by relaxing the muscles wrapped around the airways in the lungs. Imagine those airways are like tiny straws. When they get tight during an asthma or COPD flare-up, it feels like trying to breathe through a coffee stirrer. Albuterol quickly opens those straws back up, making it easier for air to move in and out. This provides almost immediate relief from symptoms like:
- Wheezing (that whistling sound when breathing)
- Coughing and a feeling of tightness in the chest
- The overwhelming feeling of not being able to get enough air
Why Is It Called a Rescue Inhaler?
The term "rescue" really says it all. This isn't a medication your loved one takes on a fixed daily schedule, like a long-term controller inhaler meant to prevent symptoms. The albuterol inhaler is specifically for those sudden, scary moments when breathing gets tough. It quite literally rescues them from immediate distress.
For caregivers, understanding this is key. When your dad says his chest feels tight, reaching for the rescue inhaler is the right move. Knowing that helps you act with confidence, which is reassuring for both of you. It’s a common need—in the United States alone, over 25 million people have asthma, making albuterol a cornerstone of respiratory care. A significant number of these fast-acting medicines are delivered via inhalers because they provide the rapid relief needed during an attack. You can find more insights on the market for these medications at Future Market insights.
Getting to Know the Device
At first glance, an inhaler can look a bit complicated, but it's really just a few simple parts working together. Taking a moment to get familiar with them will boost your confidence. You don't have to be a medical expert—just a loving partner in their care.
Before we walk through the steps, let's look at the inhaler itself. Understanding the different parts makes the whole process feel less clinical and a lot more manageable.
Anatomy of an Albuterol Inhaler
This simple breakdown of the inhaler’s components will help you quickly know what's what.
| Inhaler Part | What It Does | A Quick Tip for You |
|---|---|---|
| Metal Canister | This pressurized container holds the albuterol medicine. | Remember, this part holds the medicine and should not get wet. |
| Plastic Actuator | This is the L-shaped plastic casing that holds the canister. | It’s the part you’ll hold and clean. |
| Mouthpiece | This is the opening where the medicine comes out. | Always check inside for lint or fuzz before use. |
| Mouthpiece Cap | This cover protects the mouthpiece from dirt. | Make sure you hear it "click" back on so it doesn't get lost. |
Once you know what's what, the inhaler stops being a strange medical device and becomes just another tool you can use to help.
Taking a moment to understand each part transforms the inhaler from an intimidating medical device into a familiar and manageable tool. This simple knowledge empowers you to provide better, more assured care when it matters most.
At our core, we believe shared knowledge is the foundation of great caregiving. Helping a parent manage their health often means learning new skills and staying organized—a journey we at Don'tForgetDad are passionate about supporting. You can learn more about our mission to make caregiving less about stress and more about connection right here.
Think of it this way: learning these albuterol inhaler instructions is just another way you show up for them. The next time your loved one needs help, you'll be prepared, calm, and ready to assist them in taking that easier breath. Your confidence will be their comfort.
How to Properly Administer the Inhaler
When your loved one is struggling for breath, every second feels like an hour. Knowing exactly how to help them use their albuterol inhaler can turn a moment of panic into one of calm, controlled relief. Let’s walk through this process together, step by step, so you can feel confident and prepared when they need you.
Think of this as a supportive action, not a clinical procedure. Your calm presence is just as important as the medicine itself. We’ll cover the small details that make a big difference, ensuring each puff delivers its full, breath-restoring benefit.
Preparing the Inhaler for Use
Before you even hand the inhaler to your loved one, a little prep work is essential. This makes sure the medicine is properly mixed and ready to go. For example, imagine it’s a cool morning and your mom feels a tightness in her chest after walking to the mailbox. This is when you can step in with a steady hand.
First, remove the protective cap from the mouthpiece. It’s an easy step to forget in a hurry. It's a good habit to take a quick peek inside the mouthpiece, too, just to make sure there’s no lint or debris that could be accidentally inhaled.
Next, shake the inhaler vigorously for about 10 to 15 seconds. The medicine and the propellant inside the canister can separate over time. A good, hearty shake mixes them back together, much like you would a bottle of salad dressing. This ensures a consistent, effective dose with every puff.
Finally, if the inhaler is brand new or hasn't been used in a couple of weeks, you'll need to "prime" it. This just means getting it ready for action. Point the mouthpiece away from everyone’s face and press down on the canister to release a few test sprays—usually three or four are enough. This clears out the valve and guarantees the first puff your loved one takes is a full, proper dose.
The Gentle Art of a Calm Inhalation
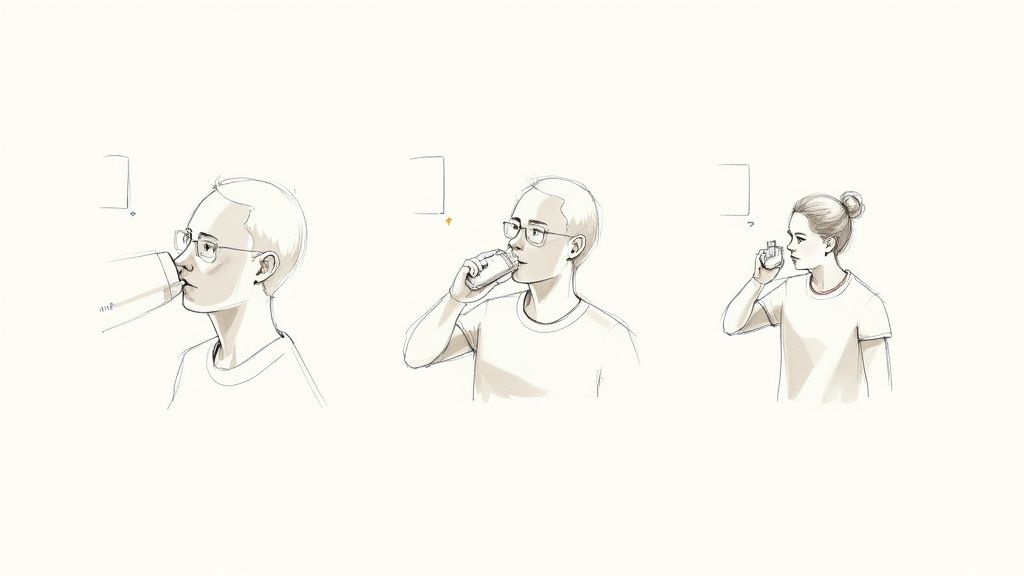
Now that the inhaler is prepped, it's time to help with the actual administration. The goal here is a slow, deep, and calm breath. Rushing can prevent the medicine from reaching deep into the lungs where it's needed most.
Have your loved one sit up straight or stand up. Good posture helps open their airways, making it much easier to take that deep, healing breath.
Next, they should breathe out fully, emptying their lungs as much as is comfortable. You can gently say, "Okay, let's blow all the air out, like you're blowing out a candle." This step makes space for the medicine to come in.
Then, they’ll place the mouthpiece in their mouth and form a tight seal with their lips. As they begin to breathe in slowly and deeply, press down firmly on the top of the canister one time. The key is coordinating that press with the very start of their slow breath in.
After the puff is delivered, they should continue breathing in for as long as they comfortably can. The next part is so important: hold their breath for up to 10 seconds. This pause is when the magic happens—it gives the albuterol time to settle in the airways and start working. After the hold, they can breathe out slowly.
A Moment of Calm: The breath-hold is arguably the most important part of the process. I’ve found that counting to 10 together, slowly and calmly, can turn this clinical step into a shared, reassuring ritual. It gives them something to focus on besides the difficulty breathing.
This whole sequence—shaking, exhaling, inhaling, and holding—is the foundation of proper inhaler use. These aren't just suggestions; clinical guidelines from organizations like the Asthma and Allergy Foundation of America confirm that these specific steps are critical for delivering the medicine effectively.
A Helpful Tool: The Spacer
Let's be honest—coordinating that "press and breathe" action can be tricky. It's especially tough for seniors, children, or anyone whose hands might be a bit shaky from arthritis. If this sounds like your situation, a spacer can be a true gift.
A spacer is just a simple, hollow plastic tube. It attaches to the inhaler on one end and has its own mouthpiece on the other. What it does is solve the coordination problem entirely.
Here’s how it works:
- Attach the inhaler to the spacer.
- Press the canister to release a puff of medicine into the chamber.
- Your loved one can then simply breathe in the medicine that’s now being held in the tube.
The spacer holds the medicated mist, allowing them to inhale it over a few normal breaths instead of one perfectly timed deep one. This simple device ensures more medicine gets to the lungs and less ends up on the tongue or at the back of the throat, which also reduces side effects like a hoarse voice.
This diagram shows the basic components you’re working with.

Understanding these three parts—the canister, the actuator, and the mouthpiece—helps demystify the device and empowers you to assist with confidence.
If you think a spacer could help, talk to your loved one’s doctor or pharmacist. They can recommend the right one and show you exactly how to use it. It's a small addition that can make a huge difference in their comfort and the effectiveness of their treatment.
Keeping the Inhaler Clean and Ready to Go
When your loved one needs their rescue inhaler, you want to know it's going to work perfectly. A clogged or dirty device is the last thing anyone needs in that moment. A little bit of simple upkeep ensures that this lifeline is clear and reliable every single time.
Think of it like this: you wouldn't want to drink from a dirty cup. A quick, weekly cleaning prevents medication from building up and blocking the spray nozzle. This simple act of care guarantees they get the full, proper dose when it matters most.
A Simple Weekly Cleaning Routine
This doesn’t have to be a big chore. All it takes is a few minutes once a week and some warm water—no special soaps or harsh chemicals needed.
First, you'll need to take the inhaler apart. Just pull the metal canister straight out of the plastic L-shaped actuator. And here’s a very important point: never put the metal canister in water. That’s where the medicine is, and it absolutely should not get wet.
Here's the simple process:
- Pop the metal canister out and set it somewhere safe and dry.
- Pull the protective cap off the mouthpiece.
- Run warm tap water through the plastic actuator for about a minute. Make sure to flush water through both the mouthpiece and the little hole where the canister normally sits.
- Shake out the extra water and let it air dry completely. This is really important. A damp actuator can get clogged just as easily as a dirty one. The easiest thing to do is just leave it on a clean towel overnight.
Once the plastic piece is completely dry, slide the canister back in, pop the cap on, and you’re all set. The inhaler is clean, clear, and ready for action.
Smart Storage for a Reliable Inhaler
Where the inhaler lives is just as important as keeping it clean. The medicine is sensitive to big temperature changes, and storing it properly is key to protecting its effectiveness.
For instance, leaving the inhaler in the car's glove compartment on a hot day can affect the pressure inside the canister, which could change the amount of medicine that comes out with each puff.
A few simple storage habits can make all the difference:
- Avoid the Car: The glove compartment is not a good home for an inhaler. It gets too hot in the summer and too cold in the winter. The inhaler should always come inside with you.
- Steer Clear of the Bathroom: The steam from showers can introduce moisture, which can lead to clogs.
- Pick a "Home Base": A bedside table, a specific kitchen drawer, or a designated pocket in a purse are all great choices. The goal is a cool, dry place where it’s always easy to find.
A consistent spot for the inhaler takes the panic out of a stressful situation. When Dad knows his inhaler is always in the top drawer of his nightstand, it offers a real sense of security and control.
Making Maintenance a Habit
Life gets busy, and it's easy for these little tasks to fall through the cracks. The trick is to tie it to a habit you already have. For example, if you organize your loved one's weekly pillbox on Sunday night, make cleaning the inhaler part of that same routine.
A recurring reminder on your phone can also be a wonderful help. For families sharing caregiving duties, a shared app helps keep everyone on the same page. If you're looking for a tool designed for exactly this kind of coordination, you might want to check out our Don'tForgetDad Android app. It's built to make these small but vital tasks simpler to manage together.
By building this small act of care into your weekly flow, you're doing more than just maintaining a piece of equipment. You're making sure your loved one has immediate, reliable access to that breath of fresh air when they need it most. That consistency is a powerful way to show you care.
Troubleshooting Common Inhaler Issues
Even when you do everything right, you might still run into a little hiccup with an albuterol inhaler. That's perfectly normal. Think of this as your gentle guide for handling those issues with a cool head, showing your loved one that you've got everything under control.
Sometimes the simplest snags cause the most stress. But knowing what to look for can turn a moment of worry into a chance to connect and show you care. You can do this.
What to Do When the Canister Feels Empty
"Is there anything left in here?" It's a question every caregiver has asked. Shaking the canister doesn't really work—that sloshing sound is often just the propellant, not the medicine. And that old trick of floating it in water? That's a myth that can actually damage the inhaler.
The only way to know for sure is the dose counter. Almost every modern inhaler has a little window on the back that shows exactly how many puffs are left.
- Make it a habit: Glance at the counter before every single use.
- Know when to refill: When that counter hits 20, it's time to call the pharmacy for a refill. Many counters even turn red to grab your attention.
- Zero means zero: If the counter reads "0," it's finished. Even if it still makes a puff sound, there’s no medicine in that spray. It's time to switch to the new one.
Trust the counter. It takes all the guesswork out of the equation and guarantees your loved one gets the dose they need, every time.
Helping When They Cough After a Puff
It's hard to watch your loved one take a puff only to start coughing right away. This happens a lot, especially when their lungs are already feeling tight and irritated. That cough is usually a sign that the medicine hit the back of their throat too fast, instead of flowing down gently into their lungs.
This is where you can be a wonderful, gentle coach. A few small tweaks can make a world of difference:
- Slow everything down. Encourage them to start breathing in a split second before they press the canister. This lets the medicine ride the wave of their breath.
- Go easy on the press. A firm, quick push is all it takes.
- Bring back the spacer. If you’re not using one, a spacer is the single best fix for this problem. It holds the medicine in a little chamber, letting them breathe it in gently over a few seconds—much easier on the airways and far less likely to cause a coughing fit.
A cough doesn't mean the dose was a total waste. Some of the medicine still got where it needed to go. The goal is just to make the next puff smoother and more comfortable.
What If No Medicine Seems to Come Out?
You press the canister down, and... nothing. No puff, no sound, no medicine. Nine times out of ten, this is a simple clog from dried medicine blocking the spray nozzle. It just means the inhaler needs a little bath.
Just follow the quick cleaning routine we talked about earlier. Pop the metal canister out (remember, never get that wet!) and run warm water through the plastic mouthpiece and case for about a minute. Let it air dry completely before putting it all back together.
This kind of simple upkeep is crucial. These little devices are the front line of defense for managing breathing issues. Albuterol metered-dose inhalers (MDIs) are a massive part of asthma and COPD treatment, with the global market valued at around $4.06 billion in 2021. It’s expected to grow to $5.32 billion by 2025 as more and more people need respiratory support. You can dive deeper into the data over at Cognitive Market Research.
Hitting a small snag with an inhaler isn't a failure. It’s just part of the journey. By knowing how to fix these common issues, you can solve them quickly and without adding to anyone's stress.
Your calm, confident response is a powerful comfort. Every time you troubleshoot a little problem, you’re doing more than just fixing a piece of plastic—you’re showing them that you're there, you're capable, and you've got their back. That's the best medicine there is.
Knowing When to Call for Medical Help
As a caregiver, you have a superpower: your intuition. You know your loved one’s daily rhythm, their good days, and the days they struggle a bit more. This insight is priceless, because while an albuterol inhaler is a wonderful rescue tool, it can't solve everything. Knowing when it's time to reach for the phone is one of the most important parts of keeping them safe.
This isn’t about creating fear. It’s about building your confidence so you can act with clarity when it counts. When you can spot the signs that more help is needed, you can move forward with a calm heart, knowing you're making the right call.
Recognizing Urgent Warning Signs
Sometimes, a breathing issue becomes too big for a rescue inhaler to handle. These are the moments you don't second-guess. If you see any of the following signs, it's time to call 911 or get to the nearest emergency room immediately.
- Breathing is fast and hard, and it doesn't slow down after using the inhaler as prescribed.
- The person is struggling to speak and can't get a full sentence out without gasping for air.
- You can see their nostrils flaring with each breath, or the muscles in their neck and between their ribs are pulling in tightly as they try to breathe.
- Their lips, face, or fingernails start to look bluish or gray. This is a major sign that their body isn't getting enough oxygen.
These symptoms mean a serious breathing crisis is happening, and it requires professional medical help right away. Trust your gut—if it feels like an emergency, it probably is.
Your job in these moments is to be their advocate and their calm in the storm. Spotting these clear signs lets you act quickly and with purpose.
When to Call the Doctor
Not every scary moment is a 911 emergency, but some patterns definitely deserve a call to their doctor. These are clues that their overall breathing condition might not be as controlled as it should be, and their treatment plan probably needs a little adjustment.
Think of yourself as a loving observer. One of the biggest clues you can gather is how often they're using that rescue inhaler.
Tracking Inhaler Usage
A rescue inhaler is for, well, rescue situations—not for everyday use. If you notice your dad, who used to need his inhaler maybe once a week, is now reaching for it several times a day, that’s a significant change.
Needing the albuterol inhaler more often is a clear signal that their underlying condition, like asthma or COPD, might be getting worse. It could mean their daily "controller" medication isn't quite enough anymore, or maybe there’s a new trigger in their environment, like pollen or dust, that’s causing flare-ups.
Give their doctor a call if you notice things like:
- Needing the rescue inhaler more than two days a week (not counting use before exercise).
- Waking up at night coughing or wheezing more than twice a month.
- You're having to refill their rescue inhaler prescription more than once every couple of months.
Jotting down a simple note of when and why they used the inhaler can be incredibly helpful for the doctor's appointment. It paints a clear picture of what’s really going on, helping the doctor make the best possible decisions for their care.
Making that call to the doctor isn't about admitting defeat; it's a proactive, loving action. It shows you’re paying close attention and are a true partner in their health.
We Hear You: Answering Your Top Inhaler Questions
When you're a caregiver, your mind is always working. You’re always thinking ahead, trying to anticipate needs and prevent problems. It's completely normal to have questions, and trust us, you're not the first to ask them. We've gathered some of the most common things we hear from families to give you the clear, straightforward answers you deserve.

How Do I Know If the Inhaler Is Empty?
This is a big one, and it’s so important. Forget the old tricks you might have heard, like shaking the canister or floating it in water. Those methods are unreliable and can actually damage the inhaler. The only surefire way to know what’s left is to use the built-in dose counter.
That little window on the back is your best friend. It tells you exactly how many puffs of medication are still inside. Get into the habit of glancing at it every single time. Once that counter hits "0," the inhaler is done. It might still make a puffing sound when pressed, but that’s just the propellant gas—there's no medicine left for your loved one.
What's the Difference Between This Blue Rescue Inhaler and Their Daily One?
It's so easy to get these mixed up, but they have completely different jobs. Think of the blue albuterol inhaler as the "rescue" medication. It works fast—within minutes—to open up the airways during a sudden breathing problem. It’s the firefighter, showing up to put out the immediate fire.
Their other inhaler, which is often a different color like purple, red, or orange, is a "controller" or "maintenance" medication. This is the one they take every single day on a schedule, even when they feel perfectly fine. It works in the background, reducing inflammation over time to prevent flare-ups from happening in the first place. This one is the fire inspector, doing the preventative work.
The blue inhaler is for right now problems. Their daily controller is for long-term prevention. Knowing this difference helps you grab the right tool for the job with confidence.
Can They Use Their Rescue Inhaler Too Much?
Yes, they can, and this is a key sign for any caregiver to watch for. Albuterol is perfectly safe when used for occasional symptoms. But if you notice your loved one is reaching for that blue inhaler more and more—maybe a few times a day instead of just a few times a week—it’s a clear signal that their underlying breathing condition isn't being managed as well as it could be.
This is your cue to call their doctor. It doesn't mean the rescue inhaler has failed; it means their overall treatment plan probably needs a tune-up. Watching how often they use it is one of the most powerful ways you can advocate for their health. For more stories and insights from fellow caregivers, the Don'tForgetDad blog is a great place to connect with others on a similar path.
Getting these details right gives you the confidence to act quickly and correctly. The care you take with their rescue inhaler can be the very thing that helps them breathe easier, day in and day out. Remember to take a deep breath yourself—you're doing a great job.
At Don’tForgetDad, our goal is to simplify the logistics of care so you can focus on what matters most: connection. Our app helps your family coordinate medication schedules with friendly reminders, keeping everyone in the loop and ensuring your loved one gets the consistent care they need to thrive. See how we help families work together at https://dontforgetdad.com.
 by Don'tForgetDad Team
by Don'tForgetDad Team